You know the feeling. Your period is a week late, then two. Your first instinct isn’t to call a doctor; it’s to call your mother or a close friend. You start with the ginger-jaggery tea (the famous kadha), you maybe try a bit of papaya, or you reach for those tiny white homeopathic pills you’ve used since childhood.
In our busy lives, we often treat an irregular cycle like a minor scheduling conflict. We tell ourselves it’s just the humidity, the commute, or that big project at work. Some of us even begin to think that having only six or seven periods a year is “just my normal.”
As a gynecologist, I want to tell you: It is time to stop guessing and start listening. While home remedies and a good diet are excellent supporting players, your menstrual cycle is the “vital sign” of your internal health. If it’s off-track, your body is trying to tell you something.
What exactly is “Normal”?
Before we dive into the why, let’s define the what. A “normal” cycle isn’t necessarily 28 days exactly.
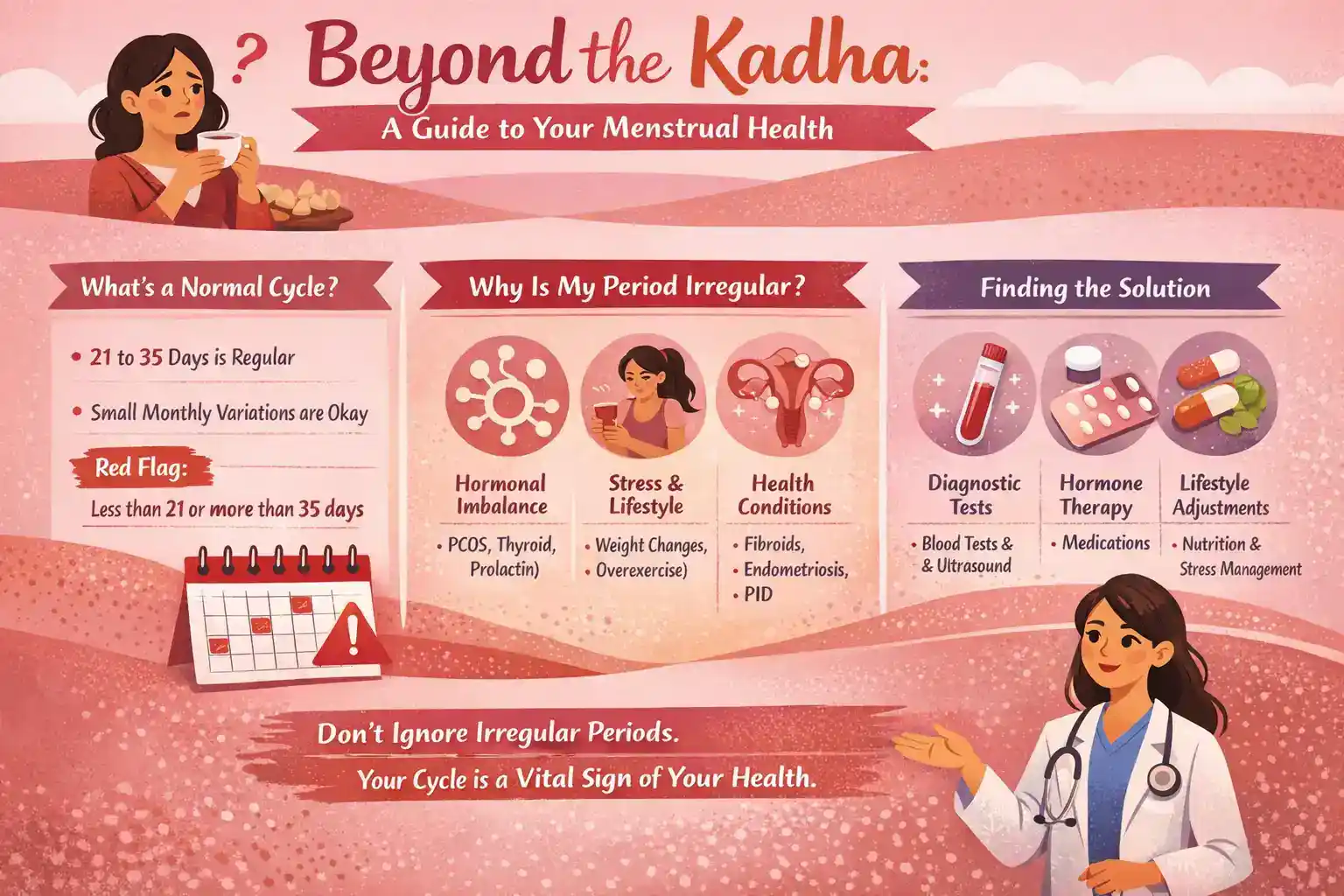
- The Window: Anything between 21 to 35 days is considered regular.
- The Variation: If your cycle varies by just a couple of days each month, you’re likely fine.
- The Red Flag: If your periods are consistently shorter than 21 days, longer than 35 days, or if the “gap” between them changes wildly every month, that is irregularity.
Why is My Cycle Off-Track? (The Deep Dive)
Irregularity is rarely about just one thing. It is usually a symphony of factors. Here are the most common medical and lifestyle reasons:
1. The Hormonal Big Three
- PCOS (Polycystic Ovary Syndrome): The most common culprit. Your body produces slightly higher levels of androgens (male-type hormones), which prevents regular ovulation.
- Thyroid Disorders: Your thyroid is your body’s “battery regulator.” If it’s underactive (Hypothyroidism) or overactive, your period is often the first thing to suffer.
- Hyperprolactinemia: This is when your pituitary gland makes too much prolactin (the milk-producing hormone), which can shut down your cycle entirely.
2. Lifestyle & Stress
- The Cortisol Effect: When you are under chronic stress, your brain produces cortisol. High cortisol tells your reproductive system, “Now is not a safe time to be fertile,” and your period simply stops or delays.
- Weight Fluctuations: Both sudden weight gain and extreme weight loss (or very low body fat) can disrupt the estrogen-progesterone balance.
- The “Overtraining” Trap: Excessive, high-intensity exercise without adequate nutrition can lead to “athletic amenorrhea.”
3. Structural & Health Conditions
- Fibroids & Polyps: These non-cancerous growths in the uterus can make periods irregular, heavy, or very painful.
- Endometriosis: When the uterine lining grows outside the uterus, it can cause significant pain and cycle disruption.
- Pelvic Inflammatory Disease (PID): An infection in the reproductive organs that often follows an untreated STI, leading to irregular bleeding.
4. The Phases of Life
- Adolescence: In the first few years after your first period, the “communication” between your brain and ovaries is still maturing.
- Perimenopause: In your 40s, as you head toward menopause, your hormone levels naturally begin to fluctuate, making cycles unpredictable.
From “Home Remedies” to Medical Care
There is a place for holistic health. Diet, yoga, and stress management are the foundation of hormonal health. However, if you have been trying home remedies for three months and your cycle is still a mystery, it is time for a professional “blueprint.”
The Danger of Waiting: Ignoring irregular periods isn’t just about a calendar. Long-term irregularity can lead to anemia (from heavy, unpredictable flow), bone density issues, and challenges with future fertility.
The Roadmap: How We Treat Irregularity
Modern gynecology is about precision. We don’t just “give you a pill”; we find the root cause.
- Diagnostic Precision: We usually start with a simple blood panel (to check Thyroid, Prolactin, and PCOS markers) and a pelvic ultrasound.
- Medical Management: * Hormonal Regulation: Low-dose birth control or progestin therapy to “reset” the cycle.
- Metformin: Often used if PCOS and insulin resistance are the cause.
- Thyroid Medication: If the “battery” is the problem, fixing the thyroid usually fixes the period.
- Surgical Options: For structural issues like large fibroids or polyps, minimally invasive (laparoscopic) procedures can remove the obstruction with very little downtime.
- Holistic Integration: We work with you to adjust your nutrition—focusing on anti-inflammatory foods, adequate protein, and “cycle-syncing” your lifestyle.
A Final Thought
You don’t have to “just live with it.” You don’t have to plan your life around the possibility of a period showing up uninvited.
Whether you are a college student, a working professional, or a busy homemaker, your health is the engine that keeps your world running. Let’s stop the guesswork and get your cycle—and your life—back on a rhythm that works for you.